Hormonal or Bacterial Acne? How to Tell the Difference
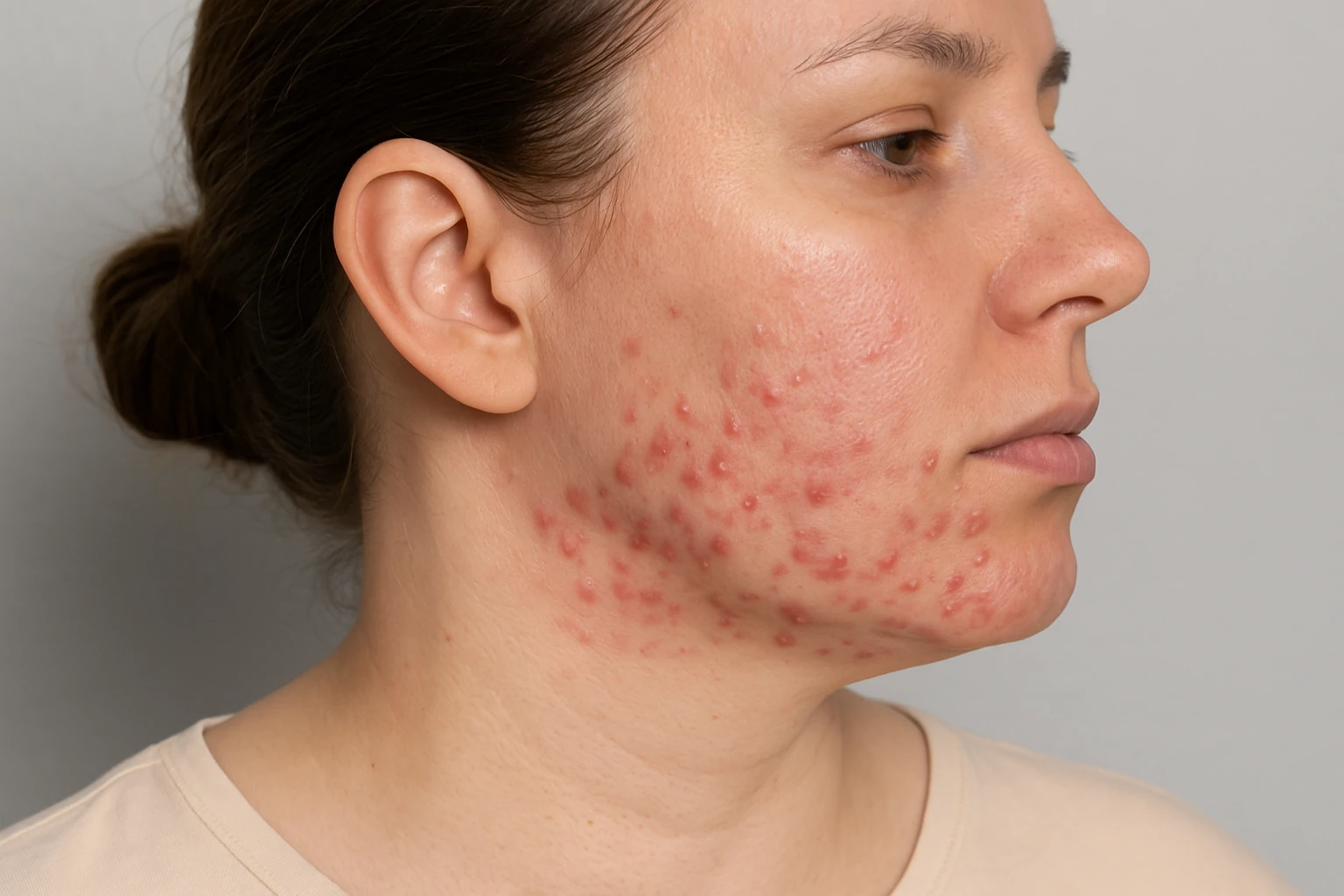
Almost everyone has dealt with acne at some point, but not all pimples are created equal. Two of the most common types are hormonal acne and bacterial acne, and telling them apart is key to choosing the right treatment.
According to dermatologists, hormonal acne often appears cyclically—around your period, during pregnancy, or during other hormonal shifts. It’s usually deeper, more painful, and shows up around the chin, jawline, or neck.
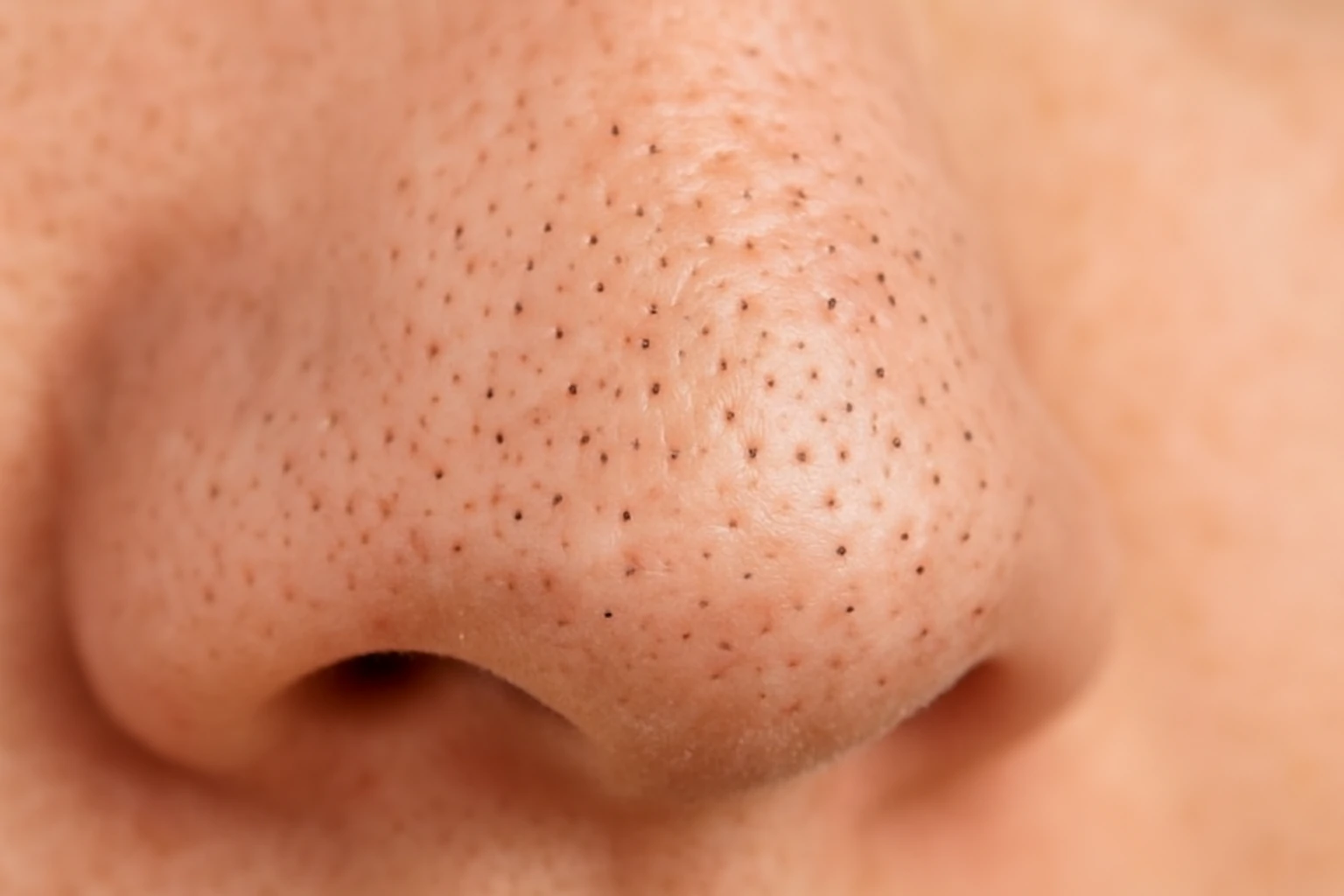
Bacterial acne, on the other hand, forms when excess oil, dead skin cells, and bacteria clog your pores. These breakouts often look like whiteheads, blackheads, or pus-filled pimples, typically showing up on oily areas of the face like the T-zone.
Understanding the difference matters. While hormonal acne may respond better to hormonal therapy or prescription treatments, bacterial acne can often be managed with the right skincare products, such as benzoyl peroxide or salicylic acid.
Spotting the right type helps you avoid wasting time (and money) on products that don’t work—and start healing your skin more effectively.
What Exactly Is Hormonal Acne?
Hormonal acne is triggered by fluctuations in hormones—especially androgens like testosterone—that cause your skin to produce more oil than it needs. This type of acne typically appears during your period, pregnancy, menopause,[1Khunger N, Mehrotra K. Menopausal acne – challenges and solutions. Int J Womens Health. 2019;11:555-567.] or conditions like PCOS (Polycystic Ovary Syndrome).
It often shows up as deep, painful bumps on the chin, jawline, neck, or cheeks. These areas are highly sensitive to hormonal changes, making them prime spots for inflammation.
What makes hormonal acne different is its cyclical pattern and its resistance to over-the-counter treatments. Dermatologists explain that when hormones spike, your sebaceous glands go into overdrive, clogging pores and encouraging bacterial overgrowth—leading to stubborn, red breakouts.
If your acne tends to follow a monthly pattern or flares up during hormonal shifts, there’s a good chance it’s hormone-related. Seeking help from a dermatologist can unlock options like topical retinoids, oral contraceptives, or even spironolactone, depending on your case.
What Is Bacterial Acne?
Bacterial acne forms when a naturally occurring skin bacteria—Cutibacterium acnes (C. acnes)—multiplies and inflames clogged pores. While this bacteria lives harmlessly on your skin, it becomes a problem when trapped with oil and dead skin.
Once inside a blocked pore, C. acnes triggers an immune response, leading to redness, swelling, and sometimes pus. This is what turns a simple clogged pore into a full-blown pimple.
Common areas for bacterial acne include the forehead, cheeks, chin, back, and chest—especially in people with oily skin.
Treating this type of acne usually involves ingredients that target both oil control and bacteria, such as benzoyl peroxide, salicylic acid, or topical antibiotics. For moderate to severe cases, dermatologists may prescribe oral antibiotics or retinoids.
By identifying and controlling the bacterial trigger, you can manage breakouts more effectively and prevent scarring.
What Causes Bacterial Acne?
Bacterial acne develops when pore blockages meet bacterial overgrowth. The main culprit, Cutibacterium acnes, feeds on trapped oil and dead skin cells—causing inflammation and visible pimples.
Key triggers that worsen bacterial acne include:
- Excess sebum production (often due to hormonal changes)
- Touching your face with unclean hands
- Wearing comedogenic skincare or makeup
- Inconsistent cleansing—especially after sweating or wearing makeup
Experts recommend maintaining a consistent skincare routine, using non-comedogenic products, and avoiding harsh scrubbing. Gentle exfoliation with salicylic acid helps keep pores clear, while ingredients like benzoyl peroxide kill bacteria.
If breakouts persist or worsen, it may be time to consult a dermatologist for targeted treatment. Understanding the root causes helps you stay ahead of flare-ups before they become chronic.
What Does Bacterial Acne Look Like?
Bacterial acne typically appears as inflamed, red pimples that may feel sore or develop a white center filled with pus. Unlike blackheads or whiteheads, these blemishes are often painful and harder to ignore.
Dermatologists describe the most common forms as:
- Papules – red, swollen bumps without visible pus
- Pustules – similar to papules, but filled with yellow or white pus
- Nodules or cysts – large, deep, and painful lumps under the skin
These lesions often show up on oily areas such as the forehead, cheeks, chin, back, or chest. Because bacterial acne involves an inflammatory process, it can also lead to post-acne scars if not treated properly.
Effective treatment targets both the inflammation and the bacteria. Topical ingredients like benzoyl peroxide, clindamycin, and retinoids are commonly recommended to reduce swelling and prevent new breakouts.
Identifying the visual signs early helps you take action before acne gets worse—or leaves long-term marks.
Is Your Acne Hormonal or Bacterial? Here’s How to Tell
Not all breakouts are the same—and knowing whether your acne is hormonal or bacterial can change everything about your skincare routine.
Hormonal acne often shows up at predictable times, like before your period or during major hormonal shifts. These breakouts tend to be deep, sore, and located around your jawline, chin, or neck. They’re triggered by hormone fluctuations, particularly an increase in androgens, which lead to oilier skin.
Bacterial acne, however, may appear more randomly and presents as blackheads, whiteheads, pustules, or even cysts. These form when pores get clogged, creating an ideal environment for C. acnes bacteria to thrive.
Dermatologists suggest a skin analysis or even hormone testing to identify the type. An accurate diagnosis is key for effective treatment.
New research also points to the importance of your skin microbiome—the balance of good and bad bacteria on your skin. Hormonal shifts can disrupt this balance, indirectly affecting bacterial growth and acne severity.
Effective Acne Treatments
Treating acne isn’t a one-size-fits-all process—it depends on what’s causing it and how severe it is. That’s why dermatologists often recommend a mix of topical and oral treatments, tailored to your unique skin type and lifestyle.
Some commonly used treatments include:
- Anti-inflammatory creams like niacinamide or low-strength hydrocortisone to calm red, irritated skin.
- Birth control pills, often prescribed for hormonal acne, help regulate androgen levels and reduce oil production.
- Topical retinoids (e.g., tretinoin) boost cell turnover, prevent clogged pores, and improve skin texture.
- Antibiotics, taken orally or applied topically, reduce bacterial infection and inflammation.
- Exfoliants like salicylic acid, glycolic acid, or benzoyl peroxide help unclog pores and control oil.
A consultation with a dermatologist is the safest route. They can recommend the right combination—without overdoing it or damaging your skin barrier.
How to Treat Hormonal Acne the Right Way
Treating hormonal acne goes beyond just applying topical products—it starts with rebalancing your hormones from the inside out.
Doctors often recommend:
- Birth control pills to regulate hormone levels and reduce sebum production.[2Del Rosso JQ, Kircik L. The primary role of sebum in the pathophysiology of acne vulgaris and its therapeutic relevance in acne management. J Dermatolog Treat. 2024;35(1):2296855.]
- Spironolactone, a medication that blocks androgen hormones, helping to calm oil glands and reduce breakouts.
- Topical treatments like retinoids, benzoyl peroxide, and salicylic acid to keep pores clear and reduce inflammation.
- A consistent skincare routine using gentle, non-comedogenic products including cleanser, moisturizer, and sunscreen.
- Lifestyle changes: Prioritize sleep, stay hydrated, reduce sugar intake, and manage stress—factors that all influence hormonal activity.
For long-term success, partner with a dermatologist who can personalize your treatment plan based on your symptoms, hormone levels, and skin sensitivity.
How to Treat Bacterial Acne Without Making It Worse
To manage bacterial acne, you’ll need treatments that clear pores and directly target bacteria without irritating your skin.
Top strategies include:
- Benzoyl peroxide – a powerful antibacterial agent that kills C. acnes and clears clogged pores.
- Topical retinoids like adapalene (Differin) – these help shed dead skin cells, reduce oil, and speed up cell renewal.
- Antibiotics, such as doxycycline or clindamycin, are used for moderate to severe bacterial breakouts but should be limited to prevent resistance.
Dermatologists recommend combining treatments—for example, using benzoyl peroxide alongside antibiotics—to improve results and avoid antibiotic resistance.
With the right routine and medical guidance, even stubborn bacterial acne can be controlled without compromising your skin’s health.
What About Fungal Acne?
Fungal acne isn’t technically acne—it’s a condition known as Malassezia folliculitis, caused by an overgrowth of yeast that naturally lives on your skin.
Unlike bacterial or hormonal acne, fungal breakouts are:
- Small, red, and itchy
- Often appear in clusters on the forehead, hairline, or upper back
- Resistant to typical acne treatments like benzoyl peroxide or antibiotics
Dermatologists recommend antifungal treatments—such as ketoconazole cream, selenium sulfide shampoo, or oral antifungals—depending on severity.
If you’ve tried acne products with no improvement and experience itching, especially in hot and humid weather, you might be dealing with fungal acne. A skin consultation is the best way to confirm and treat it effectively.
Warning Signs: When Acne Might Be More Than Just Pimples
While acne is common, certain symptoms shouldn’t be ignored—they may signal more serious skin issues or the need for medical care. Catching these signs early can help prevent long-term damage and speed up recovery.
Dermatologists recommend watching out for:
- Painful, inflamed red bumps that grow quickly
- Recurring pus-filled acne in the same area
- Cystic or nodular acne—deep, large, and hard pimples that can scar
- Acne that keeps spreading, even after using skincare products
- Dark spots or uneven skin tone that linger after breakouts
If you notice any of these, it’s a good idea to consult a dermatologist. Professional treatment can help control symptoms, prevent scarring, and improve your skin’s overall health faster than over-the-counter remedies alone.
What Makes Acne Worse? From Stress to Skincare Mistakes
Acne isn’t just caused by hormones or bacteria. External factors and daily habits can play a major role in triggering or worsening breakouts.
Dermatologists point to several common acne aggravators:
- High stress levels, which raise cortisol and increase skin inflammation
- Diets high in sugar or dairy, which can overstimulate oil glands
- Wrong skincare products, especially those that are comedogenic or high in alcohol
- Pollution and dirt, which clog pores and promote bacterial growth
- Touching or popping pimples, which can spread infection and leave scars
To prevent flare-ups, choose non-comedogenic, gentle skincare, manage stress through sleep or mindfulness, and cleanse your face consistently—especially after exposure to sweat or pollution.
How to Choose the Right Skincare for Your Acne Type
Not all acne is the same—so your skincare shouldn’t be either. Choosing the right products for your acne type makes a huge difference in how quickly your skin improves.
Here’s a quick guide recommended by dermatologists:
- Hormonal acne: Look for ingredients like salicylic acid and niacinamide to regulate oil and reduce inflammation. Retinoids are also effective for nighttime use.
- Bacterial acne: Choose products with benzoyl peroxide or topical antibiotics like clindamycin to fight infection.
- Comedonal acne (blackheads/whiteheads): Use chemical exfoliants such as AHAs or BHAs to unclog pores and renew skin.
- Cystic/nodular acne: These need medical treatment, but over-the-counter options with sulfur or retinoids can help ease inflammation.
Always pick products labeled non-comedogenic, alcohol-free, and suitable for sensitive or oily skin. A simple, targeted routine is better than overloading your skin with too many actives.
Final Thought
Understanding whether your acne is hormonal or bacterial isn’t just about labeling—it’s the first step toward real, lasting skin improvement. Each type has its own root cause, symptoms, and treatment approach, and using the wrong products can make things worse.
If your breakouts follow a pattern, feel deep and painful, or flare around your period, they’re likely hormonal. If they look red, pus-filled, or spread quickly, bacteria could be the main culprit. And in some cases, you might be dealing with fungal acne, which needs a completely different solution.
Whatever the cause, the best results come from being informed, consistent, and patient. Start by observing your skin, choosing products tailored to your acne type, and seeking help from a dermatologist when needed.
Healthy skin doesn’t happen overnight, but with the right knowledge and routine, it’s absolutely achievable.




 Acne
Acne Anti-Aging
Anti-Aging Business
Business Digital Marketing
Digital Marketing Economics
Economics Exfoliation
Exfoliation Hair Removal
Hair Removal Movies
Movies Personal Finance
Personal Finance Websites
Websites